Psoriasis of the feet is a skin disorder in which itchy papules, spots or pustules appear on certain parts of the limbs. Over time, they grow and merge into arrays. This disease is incurable and chronic. A well-designed complex therapy for rapid relief of the symptoms of foot psoriasis. Therefore, desiring to achieve stable remission (to completely or partially clear the skin from the elements of the rash), one should not appoint self-treatment.
Cause of illness
Scientists have yet to figure out why psoriasis appears on the feet and other parts of the body. Many researchers link psoriatic skin rashes with genetic breakdown in the cells of the epidermis and subsequent overactivity of the immune system. This condition occurs as follows:
- Due to the dysfunction of the skin, the keratinocytes (which make up 90% of the cells of the epidermis) do not have time to mature, but at the same time they multiply rapidly, which leads to a change in the structure of the areas. individual skin.
- In response to such a failure, the body's immunity sends T lymphocytes (killing cells) and macrophages (eating cells) to destroy the immature and replaced keratinocytes. pathological change.
- As a result of the accumulation of a large number of immune cells and keratinocytes in the upper layers of the epidermis, the skin grows and begins to peel. There is no drug that can completely normalize the functions of the skin renewal process.
The progression of foot psoriasis facilitates bacterial infections that can enter the skin through minor scratches, as well as a disturbed hormonal background, atopic dermatitis, and aother external factors.
What foot psoriasis looks like, depending on the type of disease
Psoriasis lesions on the feet and knees of the legs can look different from person to person. This factor is explained by the cyclical course of the disease. In addition, one or several forms of psoriasis can develop on the skin of the feet, including palmar, common (vulgar), teardrop-shaped, dot-shaped, as well as nail and joint psoriasis. .
Psoriasis of the legs and feet
Elements of the psoriatic rash can be localized on different parts of the skin of the legs:
- on the knee;
- on the shin;
- on the heel;
- in the thigh.
Psoriasis of the lower legs, feet, knee joints, and inner thighs begins with the appearance of single red papules and intense itching (typical for the point and gross form of the disease) or with small spotspink and purple (tear-shaped psoriasis).
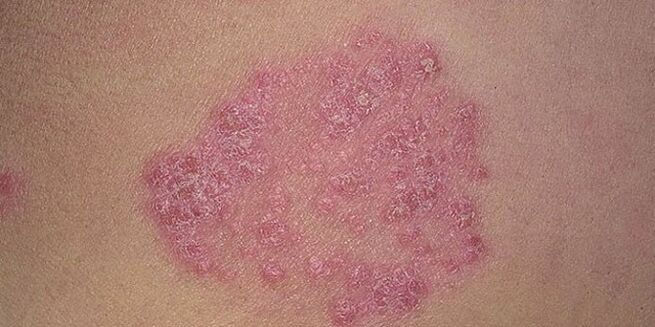
In the first case, the elements of the rash are slightly protruding above the surface of the skin, varying in density and capped with silvery scales, which flake off when scraped with the fingernails. Over time, papules increase and those that are close together merge into a single plaque. As a result, they completely cover the knee area or cover the snake skin areas from the knee to the foot. On the surface of the plates appeared peeling phenomenon.
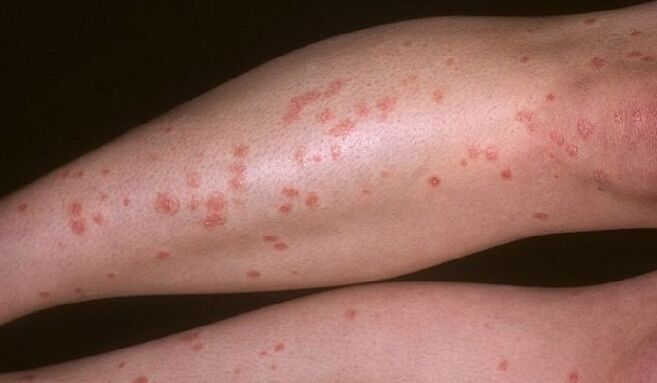
In the early stages, the teardrop-shaped elements of the psoriatic rash affect the entire skin of the feet with the same minor rash. Later, as the disease progresses, single spots form groups and cover large areas of skin on the legs. Such psoriatic lesions rarely occur on the heel.
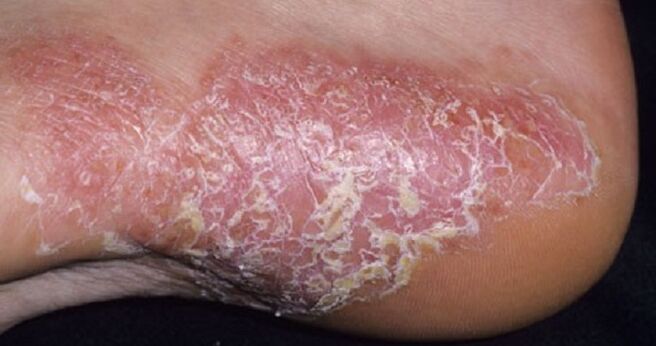
Palmar-plantar psoriasis usually develops on the soles of the feet. Elements of the rash form on the inflamed skin of the feet in the form of small spots and pustules with clear boundaries and yellow sterile content. If the pustules on the leg open, then the fluid drains out, dries up, and closes into a yellow scab, and the sores under it also dry up.
Pustules that do not burst are covered with dry scabs. Gradually, they increase and combine in clusters, the scabs begin to stretch strongly, causing discomfort when walking. The skin around the patches becomes thick and dry and cracked. Through such cracks, the infection often penetrates the deep layers of the dermis, after which the skin begins to cry and rot.
Psoriatic arthritis
In most cases, plaque psoriasis of the feet causes psoriatic damage to the joints. This arthritis is divided into 5 types:
- Symmetrical - simultaneous inflammation of the joints of the knee, hip area, ankle or foot.
- Asymmetrical - pathological changes that affect both large and small joints simultaneously, for example, the joint of one knee and the joint of the toes.
- Inflammation of the distal joints - the small joints on the toes near the nail swell.
- Osteoarthritis – Arthritis affects the entire body spine, leading to pain in the hips and lower extremities.
- Deforming arthritis is a rare inflammatory disease in which the small joints of the fingers are completely destroyed.
The skin in the joints swells, turns blue-violet and burns.
Damage to nail plates
Psoriatic nail lesions occur on the background of:
- psoriatic arthritis in 80-90% of cases;
- pustular or vulvar psoriasis in 50-60% of cases.
In 5-10% of clinical cases, toenail psoriasis is primary, i. e. it occurs on its own, without prior psoriatic involvement of the joints or skin of the feet.
Initially, psoriasis usually affects the soles of the feet or inflammatory psoriasis of the distal joints of the fingers causes pathological changes in the skin around the fingers. The pathology then spreads to the nail bed or affects the nail plate that lies on it. There is deformity of the nail - formation of indentations, cross-sections - and discoloration of the nail plate.
Similar signs of psoriasis in women are rarely observed at a young age, the disease often occurs in young men. In old age, nail damage from psoriasis affects both women and men equally.
Stages of progression
Psoriasis of the lower extremities, if left untreated, goes through 3 stages of development:
- initial;
- progressive;
- freeze.
Then the pathological changes are stopped, the period of remission begins. Without preventive treatment, the disease will recur over time.
Manifestations of the early stages of the disease in the legs are characterized by the formation of single small rash, in the form of spots, papules or pustules. At first, it can occur in both knees of both legs at the same time. The elements of the rash are red or pink, then their tops are covered with white scales. The initial stage of psoriasis lasts about 3 weeks. During this time, papules or pustules increase in size and coalesce in groups.
The initial stage of psoriasis can be stopped if you promptly seek the help of a specialist. But more often than not, people ignore the manifest symptoms of the disease, which is why psoriasis continues to develop. In the advanced stage, the number of psoriatic plaques on the skin of the feet increases, these patches are close together to form "paraffin lakes" of various shapes and sizes. Psoriasis of the toes leads to inflammation and scabbing of the tissues around the toes and damage to the fingernails.
For advanced stages, the Kebner phenomenon is characteristic, when a psoriatic rash forms on healthy skin, such as after a cut or scrape.
At the stationary stage, psoriasis of the feet and other areas of the skin on the legs still has a lot of itching and peeling. However, the new elements of the rash no longer appear and the patches stop growing in size. There is no surrounding inflammatory rim; dry scales appear in its place. If treatment is stopped at this stage, exacerbations will begin again. Otherwise, the psoriatic plaques stop flaking, some of them go away completely, some just light up - a period of remission begins.
How to treat psoriasis on feet
Foot psoriasis treatment regimens are designed for each individual patient, taking into account the location of the rash, the form of the disease, the stage of progression, and several other factors. It is very dangerous to independently invent a method of treating this disease, because complications can arise in the form of extensive skin lesions, arthritis, possible destruction, and bacterial infections (staphylococci, streptococci, etc. )bridge).
Medicine
First, the foci of psoriasis are affected by non-hormonal ointments:
- tar, naphthalan - ointments that reduce inflammation, are antiseptics, but they should be used only as prescribed by a doctor, as they have serious contraindications.
- Sulfur-salicylic ointment, salicylic acid - refers to keratolytic agents (destroys the stratum corneum). They have the effect of exfoliating and helping the plaque to disappear.
- Ointment containing solidol, softens the skin of the feet, has a regenerating effect.
- Ointments containing the active form of vitamin D3 slow down cell division, thereby reducing inflammation and flaking of the skin on the legs.
If non-hormonal drugs do not help prevent psoriasis of the legs, corticosteroid ointments are prescribed, which are divided into:
- Weak activity - the funds act on the surface of the skin, suitable for the initial stage of psoriasis. Several ointments from this group are approved for use in children, pregnant and lactating women.
- Moderately active - prescribed to treat psoriasis on rough areas of the legs, especially on the knees and soles of the feet.
- Active - prescribed if moderate ointments cannot prevent the growth of psoriatic plaques on the skin of the feet.
If no ointments for psoriasis help, then at an advanced stage of the disease, tablets are prescribed simultaneously with external drugs to:
- inhibits the activity of immune cells;
- suppresses the proliferation of epidermal cells;
- they also took retinoids - derivatives of vitamin A, which are necessary for the repair of epidermal cells.
How to get rid of psoriasis on feet with home remedies
Folk remedies for psoriasis are drugs for external use and internal use, but in the treatment of the disease should be used as carefully as drugs.
Questions like how to treat psoriasis at home well remain unanswered. Some homemade recipes help get rid of the symptoms of a long-standing disease, but not completely.
Ointment for exacerbations
Ingredient:
- unrefined sunflower oil - 1 liter;
- celandine - 50 g;
- elecampane root - 50 g;
- acetylsalicylic acid - tab 50.
Method of preparation: grind the tablets and herbs with a coffee grinder, pour the resulting powder into vegetable oil, mix well. Leave for 30 days in a warm and dark place to infuse. During this time, the mixture should be boiled every 3 days in a water bath, stirring, but not boiling.
How to use: Strain the medicine, mix the resulting solution with kerosene (3: 1), apply 3 times a day on psoriatic plaques.
Ointment relieves symptoms in 10 days
Ingredient:
- birch black - 150 g;
- medicinal alcohol - 150 mg;
- camphor oil - 75 mg;
- chicken yolk - 3 pcs.
How to cook: beat the yolk into an enameled jar, gradually add camphor, then add tar and wine. Store the ointment in a dark place.
How to use: Use a gauze pad to cover the inflamed skin on the leg. After three days, you need to wash your feet with warm water mixed with tar soap bubbles, absorb the moisture and reapply the ointment in 3 days. If the disease has not begun, then the procedure is repeated again, after which the skin is cleaned.
During treatment with homemade ointments, it is very important to maintain the body's immunity. For this purpose, it is possible to take 1 teaspoon per day. sea buckthorn oil.
Diet
Proper nutrition is one of the conditions to effectively treat psoriasis not only on the legs, but also on other parts of the body. Medical scientists conclude that allergies contribute to the development of all forms of psoriasis, so it is advisable to first exclude allergenic foods from the menu:
- egg;
- seafood;
- natural honey;
- chocolate, cocoa;
- grape;
- sheep;
- pork;
- chicken;
- alcohol.
During this period, it is very important to give up sweet, spicy, too salty and smoked foods - they slow down the metabolism in the body. The menu should include dairy products, river fish, cereals, baked apples, vegetable oils, green beans, carrots.

Complete starvation for psoriasis, when a person drinks only one water, is contraindicated.
During an exacerbation of foot psoriasis, doctors recommend arranging a fasting day once a week, such as eating only apples, kefir or boiled river fish.
Physical therapy
The answer to the question of how to treat psoriasis on the feet with physical therapy is quite extensive. For this purpose, the doctor prescribes:
- Ultrasound therapy - ultrasonic waves emitted from the device cause compression and stretching of the skin tissues, performed to restore their cells. Therefore, it is possible to reduce inflammation, itching and swelling on the skin of the feet.
- Electrosleep - prescribed for psoriasis of the skin of the feet, if a person cannot cope with the stress caused by the pathology.
- Phototherapy - under the influence of ultraviolet rays, the skin's immunity is enhanced, the rate of cell growth and division is reduced.
To improve metabolism in the skin of the legs with psoriasis, acupressure will help. It should be done only during the remission of the disease, otherwise the inflamed skin is likely to become infected.
Hygiene rules
In order not to appear new psoriasis patches on the skin of the feet, during the remission of the disease, only warm water and baby soap with moisturizing effect should be used to wash the skin of the feet. When the disease is advanced, it is advisable to wash the feet with warm water and soap for ringworm, which not only cleans the skin but also reduces inflammation. After washing, dry the skin and toenails with a soft towel.
Additional recommendations
Treatment for foot psoriasis is long-lasting if a person:
- He is engaged in an active sport - feet sweat, there is a large load on the feet. After exercising, it's important to wash your feet with warm water, dry them thoroughly, and wear clean socks and shoes that allow the skin to breathe.
- Sunbathing often and for long periods of time - too much sunbathing causes burns and depresses the skin's metabolism. In the advanced stage of psoriasis on the skin of the feet, it is better to refuse a lot of sunbathing, and in the period of remission it is recommended to use sunscreen.
Prophylactic and prognostic measures
Today, psoriasis is considered incurable. Therefore, once sustained relief of symptoms has been achieved, it is important to strive to maintain the condition in the manner recommended by the physician. There is no place for self-medication here.























